
Better Manage The Health Plan Generation Gap
Layer Personalized Health Management onto Benefits to Reflect Age Group Engagement Preferences
New research indicates that generational groups have widely varying preferences when it comes to utilizing aspects of their health plans. The differences among Millennials, Generation X and Baby Boomers when accessing benefit features argue the point that a one-size fits-all approach to employee engagement may miss opportunities to achieve savings in healthcare spend. Exploring how to layer Personal Health Management onto existing benefit plans can help optimize your members’ utilization while incenting the desired behaviors you want for better business results.
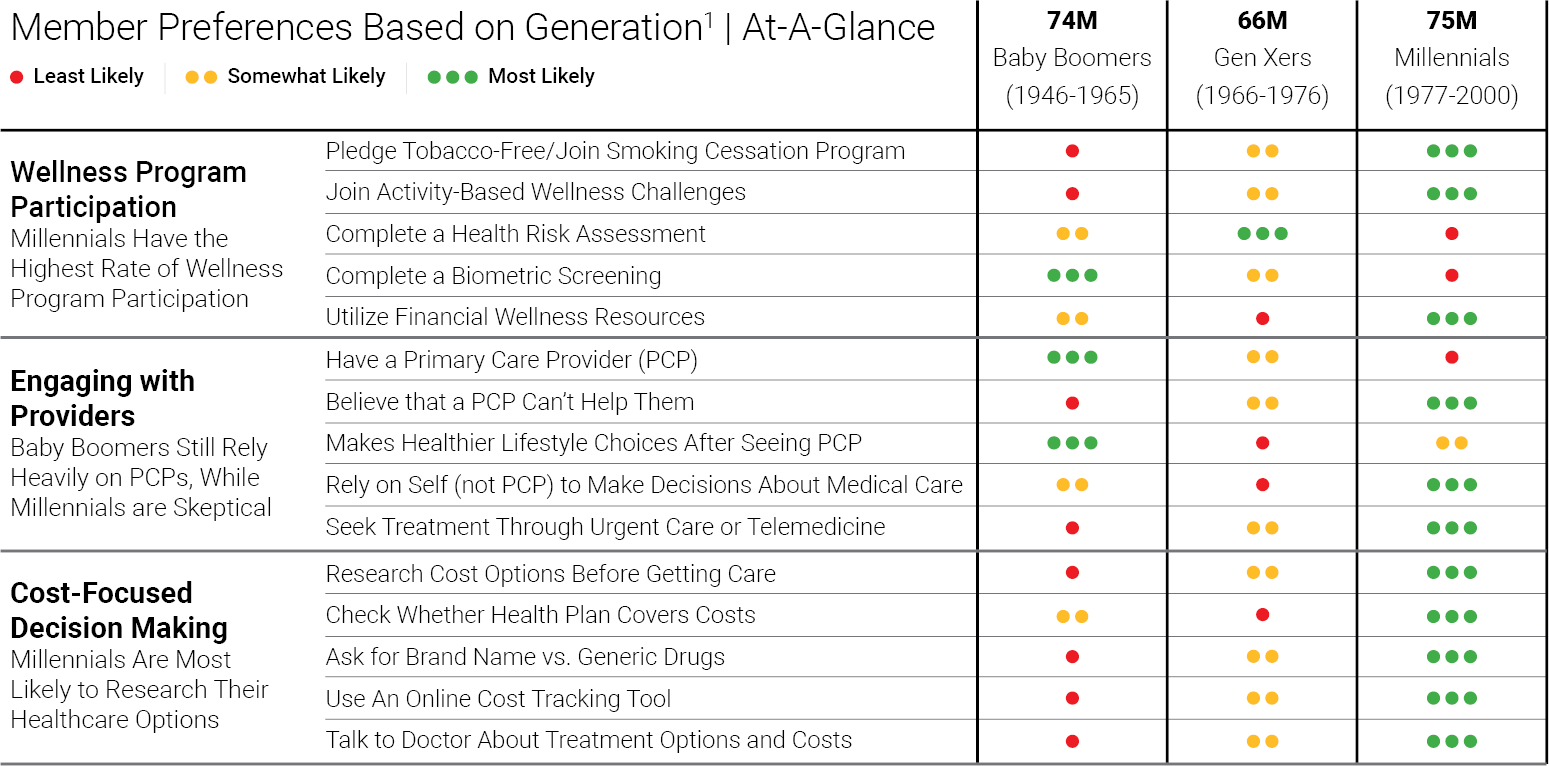
Based on a recent study1, using a primary care provider, participating in wellness programs, satisfaction with plan coverage, and proactivity in comparing costs are the key engagement differences found among generational groups seeking healthcare. If you are an employer funding health benefits, that should matter to you.
With more than 75 million individuals falling into this age category (those born 1977-2000), Millennials are on the cusp of outnumbering Baby Boomers (individuals born 1946-1965 totaling 74.9 million). Generation X (“ Gen Xers”) (those born 1966-1976), also are expected to surpass the aging Boomers in size by 2028.2
After all, across industry sectors there is a lot of interest in how Millennials shop and differ from prior generational groups given their economic force.
Meanwhile, as most Boomers reach retirement age, they represent a disproportionately large utilization of care resources. Moreover, many of them are choosing to remain working past retirement age3.
For employers seeking ways to increase benefit plan utilization and savings in healthcare claims, the study’s findings suggest that a one-size-fits all approach to engagement may miss the mark. There are distinct differences in how Baby Boomers, Millennials and Gen Xers access care treatment. Based upon your member demographics, the study reveals where certain behaviors and preferences can result in missed opportunities to influence better care decisions to drive down per-member, per-month costs.
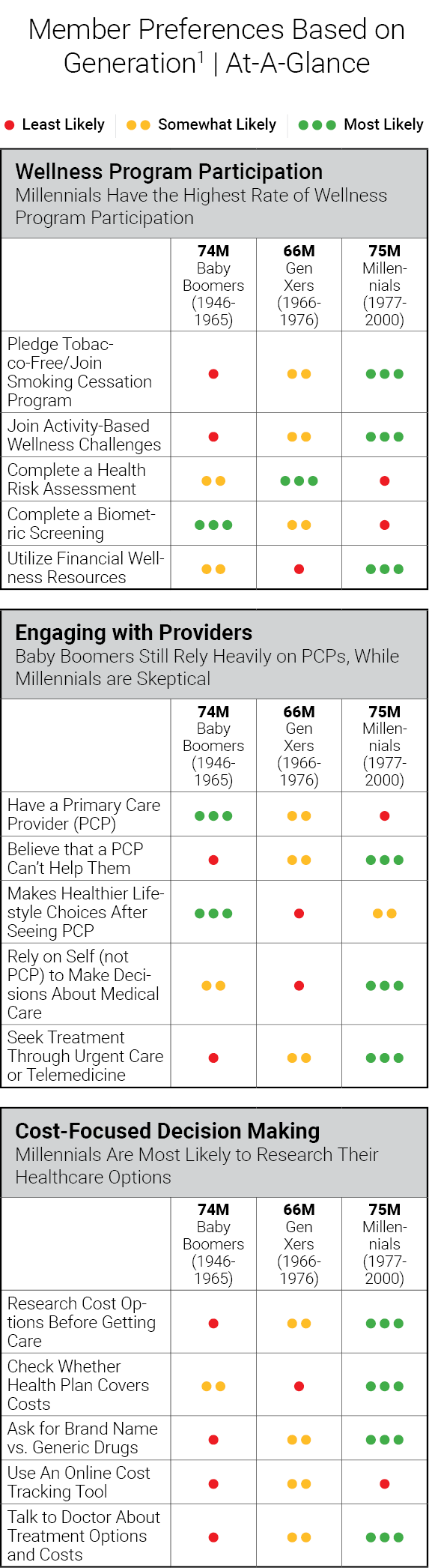

As an employer offering care benefits, your primary business goals are to a) promote health and b) minimize healthcare spend by helping people get the right care at the right time – before their conditions worsen. Many of the findings in this study point to where traditional engagement models are counter to those goals.
In the case of Millennials, their lack of value in PCPs and preference for convenience (e.g., telemedicine and urgent care) suggests greater risk for fragmented care. PCPs are trained to focus on looking at patients comprehensively and treating whole health. And while the latter options are good access points–if used solely– they run the risk of only treating immediate issues at hand, while overlooking longitudinal diagnoses and concomitant conditions.
We help employers fill-in the insight gaps to create customized plans designed to increase positive employee perceptions and better awareness and utilization of plan benefits.
Meanwhile, Baby Boomers – the age group most likely to suffer from a chronic condition – are least likely to ask questions and take a proactive approach to wellness care options.
To avoid those types of cost-increasing scenarios, it’s important to better understand your member demographics and utilization patterns. The right data analysis is the foundation to begin incenting the right care behaviors and decisions for every type of age group. Conifer Health’s Personal Health Management program has a proven track record of doing just that.
Our engagements include:
- A thorough analysis to identify members with fragmented care patterns.
- A plan of action for engagement, including positive, “stickier” relationships with a PCP – one the employee trusts – in order to reinforce the desired healthcare consumer behaviors.
- Proven programs that help individuals understand their benefits, while also coordinating their treatment services, which promotes utilization.
Conifer Health’s personalized methodology results in employee members getting the most of their benefits, while improving our clients’ cost savings through an overall healthier plan population.
References
- Ph.D. Fronstin, Paul, and Edna Dretzka. “Consumer Engagement in Health Care Among Millennials, Baby Boomers, and Generation X: Findings from the 2017 Consumer Engagement in Health Care Survey.” Employee Benefit Research Institute and Greenwald & Associates. March 5, 2018.
- Strauss, William, and Neil Howe. Generations: The History of America’s Future, 1584 to 2069. Harper Perennial, 1991.
- McGarvey, Robert. “Why Baby Boomers are not Retiring.” The Street. Feb. 27, 2016. https://www.thestreet.com/story/13474521/1/why-baby-boomers-are-not-retiring.html. Retrieved April 20, 2018.

